Introduction
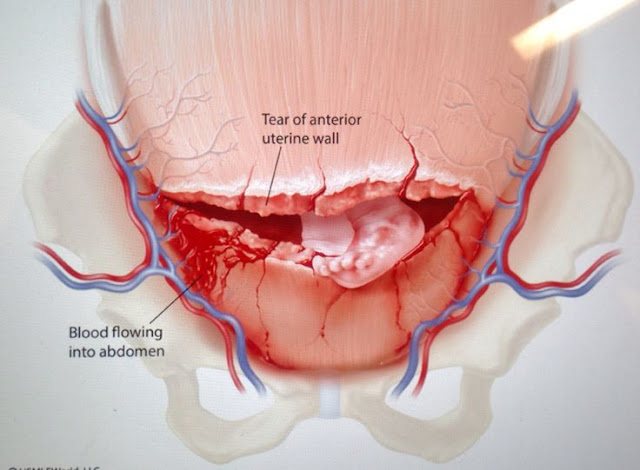
Uterine rupture is defined as a non-surgical disruption or tear of the myometrium and serosa of the uterus with or without expulsion of the fetus. It is a life threatening condition for both the mother and the fetus. The overall incidence of uterine rupture is low but in India and other developing nations, it is 10 fold higher.
Etiology
Clinical Features
USG: Fetus in peritoneal cavity, Free fluid seen
Differential Diagnosis
Management
ABC (Wide bore cannulas, fluids, O2, Blood Products)
Stop oxytocin if in progress
Type and Cross Match
Mobilising resources quickly is the key (OBGYN, Anaesthesia, Neonatology)
Immediate laparotomy is indicated
Take Home
For further reading:
Author:
Kritika Atrey
Intern
Aarupadai Veedu Medical College
Pondicherry
Twitter: @atrey_kritika
Edited by Lakshay Chanana @EMDidactic
- Scarred Uterus Rupture: Previous caesarean scar or myomectomy
- Unscarred Uterus Rupture: Obstructed labour, Trauma, Grand-multiparty, Uterine anomaly or injudicious use of oxytocin or prostaglandins
Clinical Features
- Severe haemorrhage, Tachycardia, Hypotension (Shock)
- Palpable fetal parts with loss of fetal station
- Recession of presenting fetal parts
- Prolonged, Persistent, Profound fetal bradycardia
- Loss of uterine contractility
- Hematuria
- Appearance of placenta at vulva
- Prolapsed loops of gut into vagina
Typically seen in patient with history of CS but also possible in Primigravida
USG: Fetus in peritoneal cavity, Free fluid seen
Differential Diagnosis
- Abruptio Placentae (Similar presentation)
- Hepatic Rupture in severe pre eclampsia (Look for other signs of pre-eclampsia)
- Chorioamnionitis (Look for fever, PROM, Tender uterus)
Management
ABC (Wide bore cannulas, fluids, O2, Blood Products)
Stop oxytocin if in progress
Type and Cross Match
Mobilising resources quickly is the key (OBGYN, Anaesthesia, Neonatology)
Immediate laparotomy is indicated
- Vertical incision gives better access
- Fetus lies partially or completely in the abdominal cavity
- Rent repair or hysterectomy are the surgical options depending on the degree of rupture and damage
Several studies have shown that delivery of the fetus within 10-37 minutes of uterine rupture is necessary to prevent serious fetal morbidity and mortality.
Take Home
- When dealing with trauma in pregnancy, think Placental Abruption and Uterine Rupture (Both can co-exist)
- Establishing diagnosis early and mobilising the resources quickly and effectively results in favourable outcomes for the mother and fetus
For further reading:
- Qudsia, Q. A. Z. I., et al. "Woman health; uterus rupture, its complications and management in teaching hospital bannu, pakistan." Maedica 7.1 (2012): 49.
- Blanchette H, Blanchette M, McCabe J, Vincent S. Is vaginal birth after cesarean safe? Experience at a community hospital. Am J Obstet Gynecol. 2001 Jun. 184(7):1478-84; discussion 1484-7.
- Leung AS, Leung EK, Paul RH. Uterine rupture after previous cesarean delivery: maternal and fetal consequences. Am J Obstet Gynecol. 1993 Oct. 169(4):945-50.
- Yap OW, Kim ES, Laros RK Jr. Maternal and neonatal outcomes after uterine rupture in labor. Am J Obstet Gynecol. 2001 Jun. 184(7):1576-81
- Essentials of Obstetrics - Lakshmi Seshadri and Gita Arjun
- Batra, Kanika, et al. "Determinants of rupture of the unscarred uterus and the related feto-maternal outcome: current scenario in a low-income country." Tropical doctor (2015): 0049475515598464.
- A Massinde, E Ndaboine, A Kihunrwa. An unusual case of placenta abruption complicated with ruptured uterus: case report. The Internet Journal of Gynecology and Obstetrics. 2009 Volume 13 Number 1.
Author:
Intern
Aarupadai Veedu Medical College
Pondicherry
Twitter: @atrey_kritika
Edited by Lakshay Chanana @EMDidactic